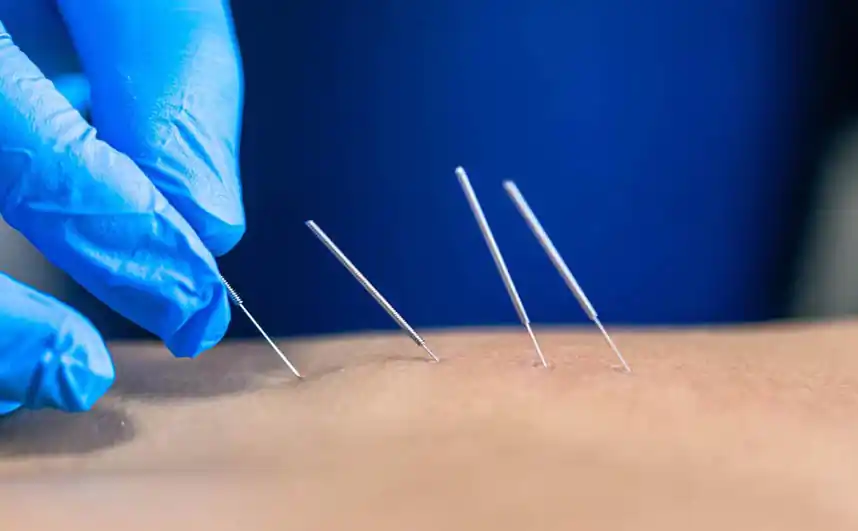
Dry needling is gradually establishing itself as an effective therapeutic technique in the treatment of musculoskeletal pain in physiotherapy. This method, which involves using fine needles to treat muscle trigger points, is appealing due to its apparent simplicity and rapid results on certain chronic conditions.
However, behind this apparent simplicity lies a complex technique that demands rigorous specialized training and a perfect mastery of safety protocols. Inserting needles into deep muscle tissue is not a trivial procedure and requires specific skills to guarantee the effectiveness of the treatment while ensuring patient safety.
This article explores the scientific basis of Dry Needling, details training requirements, analyzes potential risks, and presents best practices essential for the successful integration of this technique into modern physiotherapy.
Summary
- What is Dry Needling?
- Training and skills required
- Indications and contraindications
- Risk management and security
- Protocols and best practices
- Integration into clinical practice
- Scientific evidence and research
- Phyzio.ch: Physio software to optimize your treatments
- Conclusion
- Frequently Asked Questions
What is Dry Needling?
Dry needling, also known as dry puncture, is a modern therapeutic technique that uses sterile acupuncture needles to treat musculoskeletal disorders. Unlike traditional acupuncture, which is based on the energetic concepts of Chinese medicine, dry needling relies on rigorous Western scientific principles.
Scientific principles
This approach is based on a thorough understanding of:
- Musculoskeletal anatomy and biomechanics
- The neurophysiology of pain and modulation mechanisms
- The pathophysiology of myofascial trigger points
- Inflammatory and tissue healing processes
The technique involves precisely inserting needles into clinically identified areas of muscle tension, without injecting any substance, to obtain a local and systemic therapeutic response.
Mechanisms of action
Dry needling works through several mechanisms:
- Local muscle relaxation through direct mechanical stimulation
- Modulation of pain via neurological pathways (gate control theory)
- Improved local vascularization and tissue oxygenation
- Normalization of neurological signals to the treated muscle
Training and skills required
Professional prerequisites
Dry needling can only be performed by qualified healthcare professionals, primarily physiotherapists who have:
- A comprehensive basic training in anatomy and physiology
- Clinical experience in manual therapy
- A thorough knowledge of musculoskeletal assessment
- Skills in differential clinical reasoning
Specialized training program
A complete Dry Needling training course necessarily includes:
Theoretical foundations (40-60 hours):
- In-depth palpation anatomy and anatomical landmarks
- Neurophysiology of pain and mechanisms of action
- Pathophysiology of trigger points and myofascial syndromes
- Therapeutic indications and absolute/relative contraindications
- Security protocols and complication management
Supervised practical training (30-50 hours):
- Palpation techniques and structure identification
- Needle insertion and handling methods
- Hygiene and sterilization protocols
- Managing patient reactions and emergency situations
- Practice on anatomical models and then on volunteer patients
Assessment and certification:
- Written theoretical exam covering the entire syllabus
- Practical evaluation of technical skills
- Validation of clinical skills
- Issuance of a certificate by a recognized body
Continuing education
Mastering Dry Needling requires continuous learning:
- Regular updating of scientific knowledge
- Technical development through advanced training courses
- Participation in conferences and specialized training courses
- Exchanges with experienced practitioners
Indications and contraindications
Main indications
Dry needling demonstrates particular effectiveness in:
Muscular pathologies:
- Active and latent myofascial trigger points
- Chronic muscle contractures
- Post-traumatic muscle spasms
- Muscle overuse syndromes
Chronic pain:
- Neck and lower back pain of muscular origin
- Cervicogenic tension headaches
- Buttock pain and piriformis syndrome
- Chest pain of musculoskeletal origin
Tendon and muscle pathologies:
- Chronic tendinopathies (tennis elbow, golfer's elbow)
- Rotator cuff syndromes
- Achilles tendinitis and plantar fasciitis
- Iliotibial band friction syndrome
Absolute contraindications
Certain situations strictly prohibit the use of dry needling:
- Coagulation disorders and major anticoagulant therapy
- Severe immunosuppression and high risk of infection
- Fear of needles and severe psychological disorders
- Infected, inflamed or damaged skin areas
- Pregnancy (depending on location and trimester)
Relative contraindications
Other situations require further evaluation:
- Uncontrolled diabetes and delayed wound healing
- Immunosuppressive medications
- History of repeated vasovagal syncope
- Anatomical areas at risk (near vital organs)
- Very elderly patients or patients in poor general condition
Risk management and security
Potential risks
Although generally safe, dry needling carries inherent risks:
Immediate complications:
- Nerve damage due to improper or excessively deep insertion
- Vascular trauma and hematoma formation
- Pneumothorax during intercostal muscle treatment
- Vagal reactions and discomfort in sensitive patients
- Excessive pain and reflex muscle spasms
Delayed complications:
- Local infections due to lack of sterilization
- Persistent post-treatment pain (24-48 hours)
- Excessive inflammatory reactions
- Temporary general fatigue
Risk factors
Complications are facilitated by:
- Insufficient or inadequate training of the practitioner
- Lack of anatomical knowledge and incorrect reference points
- Failure to comply with aseptic protocols
- Insufficient clinical evaluation before treatment
- Incorrect insertion technique (angle, depth)
- Poor management of patient reactions
Prevention strategies
Security is based on:
- Comprehensive initial training and regular updates
- Systematic and rigorous clinical evaluation
- Strict adherence to hygiene protocols
- Continuous monitoring during and after treatment
- Implementation of emergency procedures
- Complete documentation of each intervention
Protocols and best practices
Pre-therapeutic assessment
Complete medical history:
- History of pain and symptomatic evolution
- Previous treatments and therapeutic responses
- Relevant medical and surgical history
- Current medications and known allergies
- Psychosocial factors and patient expectations
Clinical examination:
- Postural assessment and movement analysis
- Muscle palpation and trigger point identification
- Safety neurological and vascular tests
- Pain assessment (validated scales)
- Objective functional measures
Information and consent
Patient information:
- Clear explanation of the technique and objectives
- Description of the sensations expected during treatment
- Information on expected benefits and timeframes for action
- Presentation of possible risks and their management
- Available therapeutic alternatives
Informed consent:
- Sufficient time for the patient to reflect
- Answers to all questions asked
- Collection of written and dated consent
- You can withdraw your consent at any time.
Treatment protocol
Preparation :
- Comfortable and secure patient setup
- Adequate exposure of the area to be treated
- Skin disinfection with antiseptic solution
- Preparation of sterile equipment (needles, gloves)
Insertion technique:
- Precise anatomical identification and palpation
- Gradual insertion with appropriate angle and depth
- Monitoring of patient reactions
- Manipulation according to the therapeutic objective
- Safe removal and hemostasis control
Post-treatment monitoring:
- Patient observation for 15-20 minutes
- Checking for the absence of complications
- Management of potential side effects
- Advice for the following hours
- Planning of therapeutic follow-up
Clinical documentation
Patient file:
- Detailed record of the initial assessment
- Precise description of the treated areas
- Technical parameters used (depth, duration)
- Patient reactions and immediate response
- Treatment plan and objectives set
Integration into clinical practice
Multidisciplinary approach
Dry needling integrates optimally into a comprehensive therapeutic approach:
- Coordination with prescribing physicians
- Collaboration with other professionals (osteopaths, massage therapists)
- Integration into a comprehensive rehabilitation program
- Follow-up care shared with the healthcare team
- Regular communication on developments
therapeutic combination
The effectiveness of Dry Needling is enhanced by:
- Manual therapy: joint mobilizations and manipulations
- Therapeutic exercises: specific strengthening and stretching
- Patient education: understanding their condition
- Ergonomics: adapting the workstation and habits
- Stress management: relaxation and mindfulness techniques
Cabinet organization
Successful integration requires:
- Staff training on specific protocols
- Appropriate equipment and maintenance of sterilization
- Appropriate professional liability insurance
- Clearly defined emergency procedures
- Monitoring of staff training and certifications
Scientific evidence and research
Current data
Research on Dry Needling is experiencing significant development:
- Randomized controlled trials are increasing
- Meta-analyses confirming effectiveness on certain pathologies
- Research on neurophysiological mechanisms of action
- Comparisons with other therapeutic techniques
- Safety and tolerability studies
Limitations and perspectives
The research still identifies needs:
- Standardization of treatment protocols
- Identification of optimal responder patients
- Determining the ideal technical parameters
- Evaluation of long-term effectiveness
- Comparative health economics studies
Phyzio.ch: Physio software to optimize your treatments
Integrating dry needling into your clinical practice requires optimal management of patient records, schedules, and therapeutic documentation. Phyzio.ch is a Swiss physiotherapy software specifically designed to support physiotherapists in their daily practice.
This software offers:
- Complete management of patient files with detailed documentation of Dry Needling sessions
- Optimized appointment scheduling with automatic reminders (SMS, email)
- Personalized therapeutic monitoring and evaluation of results
- Billing in accordance with Swiss rates and insurance management
- Secure interface compliant with data protection standards
With Phyzio.ch, you can precisely document your dry needling treatments, track your patients' progress, and optimize your administrative organization. This solution allows you to focus on what matters most: the quality of care and therapeutic support for your patients.
To discover how Phyzio.ch can improve your Dry Needling practice, visit: https://phyzio.ch/fr/logiciel-physio .
Conclusion
Dry needling represents a valuable therapeutic complement in the modern physiotherapist's arsenal. Its proven effectiveness in treating myofascial pain and musculoskeletal dysfunctions makes it a sought-after tool for patients and appreciated by practitioners.
However, this technique cannot be mastered without a significant investment in training and supervised practice. The anatomical complexity, potential risks, and the need for rigorous clinical evaluation make dry needling a specialized medical procedure that allows for no approximations.
The success of its integration rests on several fundamental pillars: comprehensive initial training, continuous knowledge updating, strict adherence to safety protocols, and a patient-centered approach. Practitioners who embark on this path must be prepared to dedicate the time and resources necessary for a complete mastery of this technique.
When performed under these optimal conditions, dry needling significantly expands the therapeutic possibilities of contemporary physiotherapy, offering patients effective solutions for often complex and debilitating pain. Its future looks promising, driven by dynamic research and growing recognition of its clinical value.
Frequently Asked Questions
What is the difference between dry needling and acupuncture?
Traditional acupuncture is based on the energetic principles of Chinese medicine and meridians, while Dry Needling is based on Western anatomy and neurophysiology, specifically targeting muscular trigger points and neuromuscular dysfunctions.
Is dry needling painful?
The sensation varies depending on the patient and the areas treated. Needle insertion usually causes minimal sensation, but hitting the trigger point can trigger a brief muscle contraction and characteristic referred pain, a sign of the treatment's effectiveness.
How many sessions are needed?
The number of sessions depends on the condition, the duration of symptoms, and individual response. Generally, improvement is felt from the first sessions, and a cycle of 3 to 6 treatments spaced one week apart allows for an assessment of effectiveness.
What are the possible side effects?
Side effects are generally mild: temporary local pain (24-48 hours), fatigue, and slight bruising at the insertion point. More serious complications (infections, nerve damage) are rare with proper technique.
Who can practice Dry Needling?
Dry needling should be performed exclusively by qualified healthcare professionals (physiotherapists, physicians) who have completed certified specialized training. A solid foundation in anatomy and clinical experience are essential.
Does Dry Needling replace other treatments?
No, dry needling is a complementary therapy that is part of a comprehensive approach including manual therapy, exercises, patient education, and lifestyle modifications. Its effectiveness is optimized by this multidisciplinary approach.
Are there any absolute contraindications?
Yes, particularly coagulation disorders, severe immunosuppression, needle phobia, infected areas, and certain pregnancy situations. A prior clinical evaluation can identify these contraindications.